Degenerative Knee Repair
Without Surgery
What Are ACL/PCL And Meniscal Tears?
The knee is the largest joint in the body and is one of the strongest (See Figure 1). It’s composed of three bones: the bottom part of the thighbone, called the femur; the top part of the shinbone, called the tibia; and a large, round bone that covers and protects the joint, called the patella or kneecap.
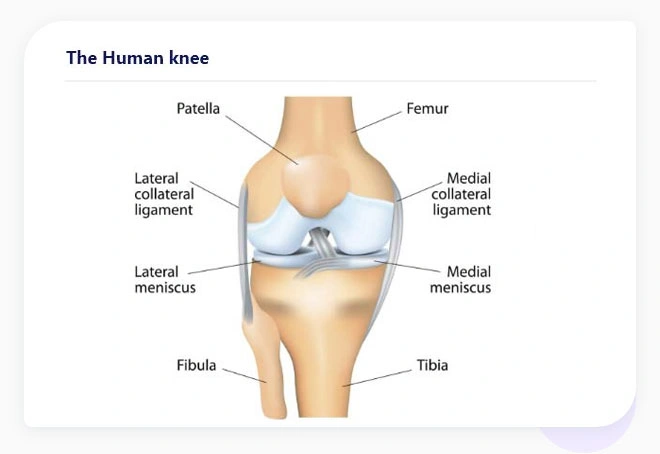
Figure 1. Shown is the knee joint composed of the femur, tibia, and patella (kneecap). Several ligaments including the ACL and PCL provide support to the knee, holding the bones in the proper alignment. The knee is also composed of two critically important tendons, strong fibrous connective tissue that serve to hold bones together. These tendons are the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL). The ACL prevents the tibia from sliding forward along the femur, while the PCL prevents the tibia and femur from sliding backward.
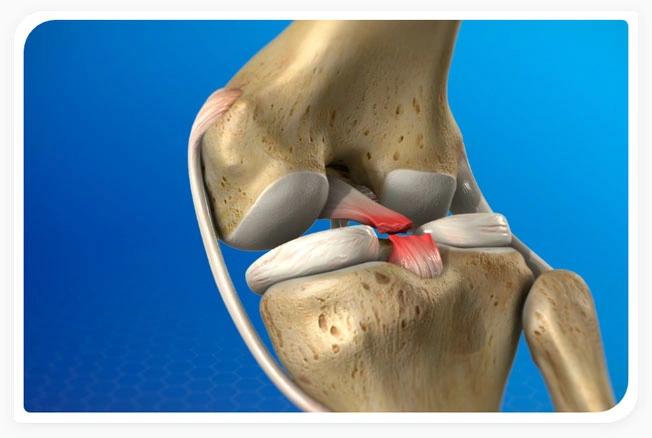
The ACL and PCL can tear or rupture in the knee (See Figure 2) when stretched too far by landing on the leg when the foot is turned or by trauma to the knee. ACL and PLC tears in the knee occur most commonly in young and active individuals and can have negative long-term physical impacts.
Figure 2. The human knee is composed of two crossing ligaments called the anterior (ACL) and posterior cruciate ligaments (PCL). Both ligaments provide rotational stability to the knee. An example of an ACL tear is shown in (A) magnified in the circle. Similar injuries can be observed in the PCL (B).
Without the proper support of the ACL and PCL, the knee can become painfully unstable and the articular cartilage covering the bones in the knee can wear down over time causing osteoarthritis in the joint (see Figure 3).
Osteoarthritis of the knee is a progressive condition that causes aching pain, stiffness, and loss of mobility in the knee joint. The cause of knee pain and other osteoarthritis symptoms is often bone-on-bone friction related to “wear and tear” of the cartilage in the affected joint.
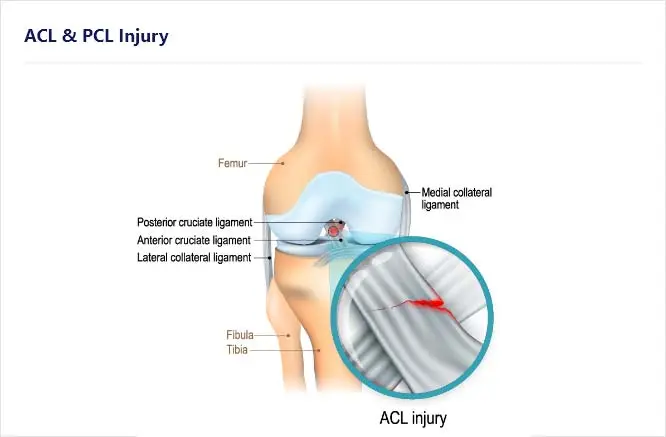
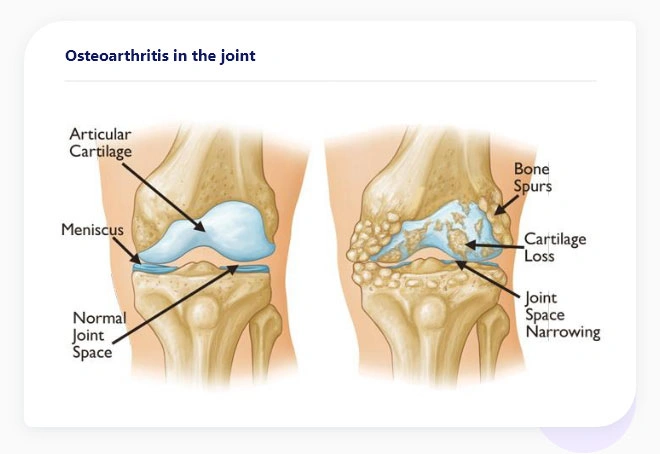
Figure 3. (left) Depiction of a normal knee joint. Note the amount of joint space and smooth surface of the articular cartilage in the normal knee. (right) Depiction of osteoarthritic knee with articular cartilage loss, bone spurs, and narrowing of the joint space.
Causes, Signs And Symptoms
What are the symptoms of ACL/PCL and meniscus damage?
Patients with ACL and PCL tears or ruptures in the knee may experience one or more of the following symptoms:
- Sharp or dull pain behind the knee (PCL tear)
- Popping sound at time of injury (ACL)
- Severe pain and inability to continue activity
- Rapid swelling and/or bruising
- Loss of range of motion
- A feeling of instability or “giving out” with weight bearing
- Warm to the touch, tenderness, numbness

What are risk factors for ACL/PCL and meniscus injuries?
ACL and PCL tears are most often activity related by have other contributing factors including:
Age. ACL and PCL tears are most common in those 15-45 years of age due to their more active lifestyles and participation in sports.
Gender. Females have a higher incidence of ACL and PCL injuries relative to males, possibly due to differing bone shapes at the point of ligament attachment, wider pelvis, greater ligament laxity, and neuromuscular factors.
High-risk Sports. ACL and PCL tears occur most often in sports that require frequent or sudden deceleration, cutting, pivoting, or landing on one leg (e.g., downhill skiing, lacrosse, tennis, basketball, soccer, football, and volleyball).
Previously Torn ACL or PCL, the risk of re-tearing a previously repaired ACL/PCL is up to 20% higher.
How are ACL/PCL and meniscus tears diagnosed?
Our specialists base their diagnosis of ACL and PCL tears using a multipronged approach:
- Medical History: Our doctors will ask you about the nature of your knee pain (e.g., when and under what conditions you experience knee pain). They will ask about prior surgeries, accidents, and trauma to the knee.
- Physical Exam: The doctor will check for signs of trauma by testing the range of motion and listening for any cracking or popping noises (crepitus) or tenderness/pain, bruising, and swelling.
- Magnetic resonance imaging (MRI): This imaging test shows a detailed view of the ligaments surrounding the knee joint and is the only way to confirm diagnosis of ACL and PCL tears/ruptures. X-rays cannot show tears but can rule out other sources of knee pain.
Treatment Options
How are knee meniscus tears treated?
The StemX clinic offers a range of customized Regenerative Medicine treatments to treat orthopedic injuries.
Wharton’s Jelly
PRP
Hyaluronic Acid/
Prolotherapy
The StemX Approach
StemX is California’s leading provider of holistic and regenerative medicine services. Our experts don’t just offer popular treatments, but customized medical solutions based on individual needs.
Located in Solana Beach, California, the StemX clinic is composed of a team of expert doctors with years of experience administering regenerative medicine treatments for joint disease. Our team has:
How To Get Started
Consultation:
Our California-based clinic intake team will match you to the appropriate provider with the expertise to treat your injury and schedule an exam.
Initial Exam:
Your doctor will take your medical history and facts surrounding your injury/complaint, conduct a physical exam, and order imaging tests (X-rays, MRI’s, etc.).
Treatment determination:
Use this space to add a short description. It gives enough info to earn a click.
Mark your calendar:
A date will be set for your procedure, and you will be given instructions on how to prepare for your appointment.
Treatment Procedure
While each treatment may be customized, you can expect your experience to be similar to the following:



