Treat Chondromalacia Naturally Without Steroids or Surgery
What Is Chondromalacia?
Chondromalacia patellae, also known as “runner’s knee,” is a condition where the articular cartilage on the underside of the patella or kneecap deteriorates and softens. This condition is common among young, athletic individuals, but may also occur in older adults who have osteoarthritis of the knee.
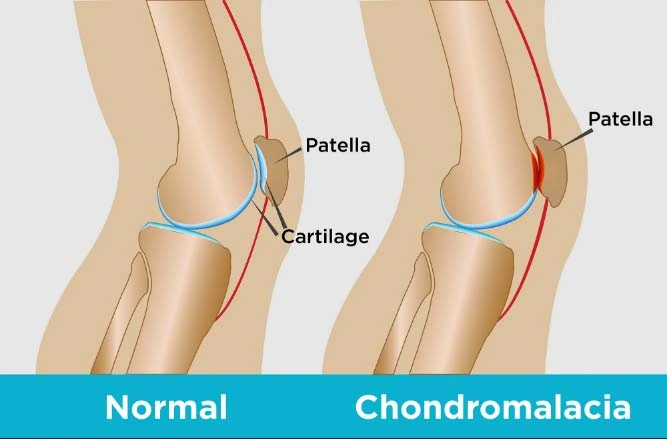
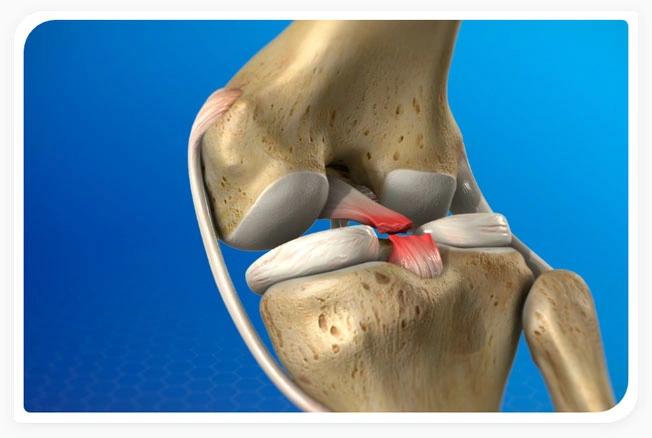
The patella sits between the femur (upper leg bone) and tibia (shinbone) residing over the front of the knee joint. The patella not only protects the knee joint but connects muscles in the front of the femur to the tibia. Under the patella and the at the end of the femur is articular cartilage, which makes it possible for the patella and femur bones to move alongside each other without friction. When these components fail to move properly, it can cause the kneecap to rub against the femur causing the patellar cartilage to wear down causing symptoms typical of chondromalacia.
Causes, Signs And Symptoms
What are the symptoms of chondromalacia?
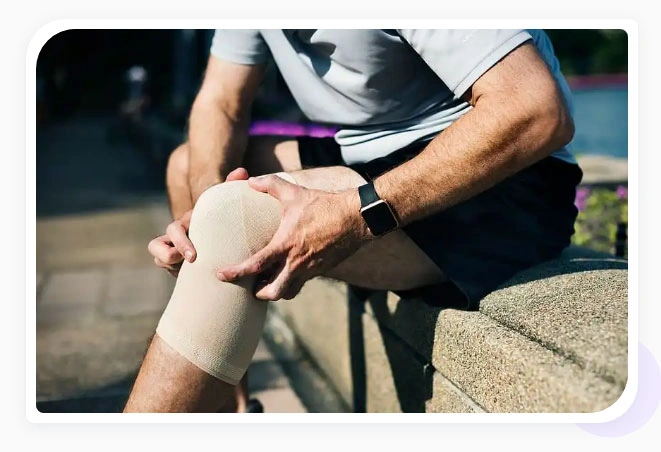
Symptoms of Chondromalacia will typically present as pain in the knee region, known as patellofemoral pain. Most common symptoms of this condition are:
- Pain behind kneecap (patellofemoral syndrome pain or kneecap pain)
- Grinding or cracking when bending/extending the knee (kneecap popping)
- Kneecap pain when walking or standing for long periods
- Warmth, tenderness, swelling. This can also be associated with patellar bursitis which often accompanies chondromalacia

What are the causes of chondromalacia?
Knee cap pain or patellofemoral syndrome pain typical of Chondromalacia are caused by various musculoskeletal imbalances including the following:
A direct blow or trauma to your kneecap
Poor knee alignment due to a congenital condition
Weak hamstrings and quadriceps (the muscles in the back and front of your thighs, respectively)
Muscle imbalance between the adductors and abductors (the muscles on the outside and inside of your thighs)
Repeated stress to your knee joints, such as from running, skiing, or jumping
Causes, Signs And Symptoms
What are risk factors for chondromalacia?
Chondromalacia can affect the young and old. Here are the most common risk factors:
- Age. Adolescents experiencing growth spurts can cause muscles and bone to develop rapidly creating short-term imbalances.
- Sex. Females are at higher risk as they typically possess less muscle mass than males causing abnormal knee positioning.
- Flat feet. More stress is placed on the knee due to flat feet relative to higher arches.
- Activity level. Frequent, repetitive, high impact activities increase the risk for knee problems.
- Arthritis. Chondromalacia can be a symptom of osteoarthritis where inflammation alters the function of the knee.
How is chondromalacia diagnosed?
Our specialists base their diagnosis of Chondromalacia (Patellofemoral Syndrome) using a multipronged approach:
- Medical History: Our doctors will ask you about the nature of your knee pain (e.g., when and under what conditions you experience knee pain). They will ask about prior surgeries, accidents, and trauma to the knee.
- Physical Exam: The doctor will assess your knee function by testing the range of motion, pain when kneeing, listen for any cracking or popping noises (crepitus), and perform a patellar grind or Clark’s test to test for chondromalacia.
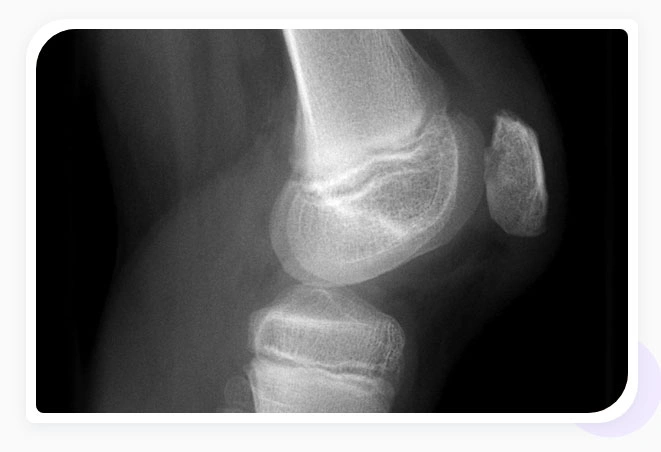
- Imaging with X-Rays or MRI: X-rays can diagnose osteoarthritis of the knee which can co-occur with chondromalacia but are not sufficient to diagnose chondromalacia. Blood tests can rule out other forms of arthritis. More advanced imaging like magnetic resonance imaging (MRIs) will be required to determine the extent of damage to the knee.
- Arthroscopy: A tiny, flexible camera can be inserted into the knee to determine the condition of the cartilage.
How are ACL/PCL and meniscus tears diagnosed?
Our specialists base their diagnosis of ACL and PCL tears using a multipronged approach:
- Medical History: Our doctors will ask you about the nature of your knee pain (e.g., when and under what conditions you experience knee pain). They will ask about prior surgeries, accidents, and trauma to the knee.
- Physical Exam: The doctor will check for signs of trauma by testing the range of motion and listening for any cracking or popping noises (crepitus) or tenderness/pain, bruising, and swelling.
- Magnetic resonance imaging (MRI): This imaging test shows a detailed view of the ligaments surrounding the knee joint and is the only way to confirm diagnosis of ACL and PCL tears/ruptures. X-rays cannot show tears but can rule out other sources of knee pain.
Treatment Options
How is chondromalacia treated?
The StemX clinic offers a range of regenerative medicine advanced therapy treatments to treat orthopedic injuries.
Wharton’s Jelly
PRP
Hyaluronic Acid/
Prolotherapy
The StemX Approach
StemX is California’s leading provider of holistic and regenerative medicine services. Our experts don’t just offer popular treatments, but customized medical solutions based on individual needs.
Located in Solana Beach, California, the StemX clinic is composed of a team of expert doctors with years of experience administering regenerative medicine treatments for joint disease. Our team has:
How To Get Started
Consultation:
Our California-based clinic intake team will match you to the appropriate provider with the expertise to treat your injury and schedule an exam.
Initial Exam:
Your doctor will take your medical history and facts surrounding your injury/complaint, conduct a physical exam, and order imaging tests (X-rays, MRI’s, etc.).
Treatment determination:
Use this space to add a short description. It gives enough info to earn a click.
Mark your calendar:
A date will be set for your procedure, and you will be given instructions on how to prepare for your appointment.
Treatment Procedure
While each treatment may be customized, you can expect your experience to be similar to the following:



