Treat Foot Pain Naturally
with Regenerative Medicine
What is Foot Pain?
Damage to the bones, joints, ligaments, or tendons in the foot can cause significant pain. Most foot pain is the result of either trauma, overuse, or inflammatory conditions.
Causes, Signs And Symptoms of Foot Pain
What are the causes of foot pain?
One common cause of foot pain is osteoarthritis (OA). OA involves the progressive breakdown of articular cartilage that permits bones to slide past each other at joints (see Figure 1).
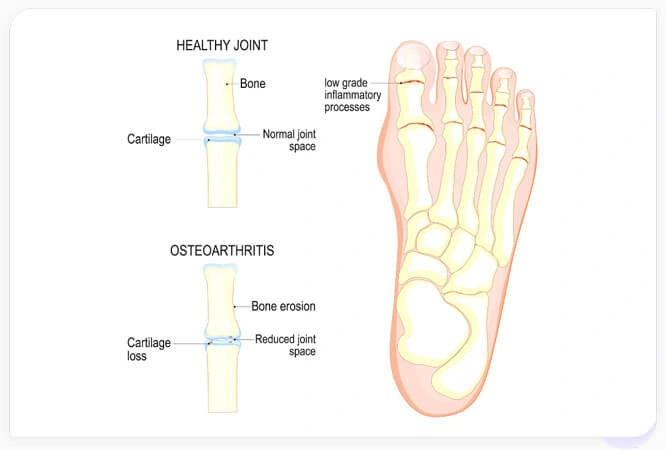
Figure 1: Depiction of foot osteoarthritis. Healthy joints have intact articular cartilage and space between opposing bones in a joint. Arthritic joints have damaged cartilage on each bone that increases the friction between due to decreased joint space.Other types of foot pain include:
Foot tendonitis: Inflammation of any of the tendons in the foot can cause foot pain (e.g., Achilles tendonitis, extensor tendonitis, peroneal tendonitis, posterior tibial tendonitis, plantar fasciitis)
Pain on top of the foot: caused by tight-fitting shoes, or overuse of tendons along the top of the foot pulling the foot upwards.
Bone spurs: Osteophytes or bony growths can form on the bones in the heel and toes.
What are symptoms of foot pain?
Symptoms of foot pain vary in location (top, side, or bottom of the foot) and according to the cause. Symptoms of foot osteoarthritis include:
- Crepitus: crunching, popping, or grating noises coming from the joints in the feet
- Pain: dull aching pain especially after activity or wearing uncomfortable shoes
- Joint stiffness
- Joint swelling
- Decreased mobility
- Pain in the first joint that connects the big toe to the foot or in the midfoot
Symptoms of foot tendonitis include:
Heel pain
Pain from bone spurs
Pain following the length of the tendon
Pain at the attachment point of the tendon to the bone
Tendon stiffness when waking up in the morning or after inactivity


Risk factors for foot osteoarthritis and other foot pain:
- Age. Changes in the cells and extracellular matrix of joint tissues that occur in aging increase the susceptibility of older adults to OA, in addition to more wear and tear over time.
- Sex. Women are more likely to develop osteoarthritis, this may be related to age-related nutritional deficiencies and hormonal changes (e.g., menopause).
- Obesity. Being overweight places excess burden on the body’s joints and may increase the pace of cartilage degeneration as does a sedentary lifestyle.
- Repeated stress on the joint. Repetitive activities can damage tendons and ligaments and lead to more wear and tear in joints. This can involve activities related to one’s profession or sporting activities.
- Previous trauma. Trauma to ligaments and tendons in the ankle or to the bones increase the risk for OA.
- Genetics. There is a higher risk of developing OA if it runs in the family.
- Bone deformities. Abnormal bone structure increases the stress at joint, muscles, tendons, ligaments contributing to OA, tendonitis, and bursitis.
- Metabolic diseases. Changes in the mineral content and health of the tissues and bones in the foot that can lead to increased risk for OA.
How is foot pain diagnosed?
Our specialists diagnosis foot pain by using a multipronged approach:
Imaging with X-Rays or MRI: X-rays and magnetic resonance imaging (MRIs) are used to determine if your foot pain is due to arthritis, fractures, heel spurs, loss of fatty pad tissue under the heel, or damage to tendons and ligaments.
Medical History: Our doctors will ask you about the nature of your foot pain (e.g., when and under what conditions you experience foot pain). They will ask about prior surgeries, accidents, and trauma to the foot, ankle, and leg.
Physical Exam: The doctor will examine the range of motion of the foot, look for swelling and muscle/tendon tightness.

Treatment Options
How does StemX How does StemX treat degenerative issues associated with foot pain?
The StemX clinic offers a range of customized Regenerative Medicine treatment solutions for foot pain.
Wharton’s Jelly
PRP
Hyaluronic Acid/
Prolotherapy
The StemX Approach
StemX is California’s leading provider of holistic and regenerative medicine services. Our experts don’t just offer popular treatments, but customized medical solutions based on individual needs.
Located in Solana Beach, California, the StemX clinic is composed of a team of expert doctors with years of experience administering regenerative medicine treatments for joint disease. Our team has:
How To Get Started
Consultation:
Our California-based clinic intake team will match you to the appropriate provider with the expertise to treat your injury and schedule an exam.
Initial Exam:
Your doctor will take your medical history and facts surrounding your injury/complaint, conduct a physical exam, and order imaging tests (X-rays, MRI’s, etc.).
Treatment determination:
Use this space to add a short description. It gives enough info to earn a click.
Mark your calendar:
A date will be set for your procedure, and you will be given instructions on how to prepare for your appointment.
Treatment Procedure
While each treatment may be customized, you can expect your experience to be similar to the following:



